Abstract
Acute gastroenteritis is common in childhood. The estimation of the degree of dehydration is essential for management of acute gastroenteritis. Plasma water was assessed as a diagnostic tool in children with acute gastroenteritis and dehydration admitted to hospital. In a prospective cohort study, 101 patients presenting at the emergency department with dehydration were included. Clinical assessment, routine laboratory tests, and plasma water measurement were performed. Plasma water was measured as a percentage of water content using dry weight method. During admission, patients were rehydrated in 12 h. Weight gain at the end of the rehydration period and 2 weeks thereafter was used to determine the percentage of weight loss as a gold standard for the severity of dehydration. Clinical assessment of dehydration was not significantly associated with the percentage of weight loss. Blood urea nitrogen (r = 0.3, p = 0.03), base excess (r =−0.31, p = 0.03), and serum bicarbonate (r = 0.32, p = 0.02) were significantly correlated with the percentage of weight loss. Plasma water did not correlate with the percentage of weight loss. On the basis of the presented data, plasma water should not be used as a diagnostic tool in the assessment of dehydration in children with acute gastroenteritis.
Similar content being viewed by others
Introduction
Dehydration is the most important complication of acute gastroenteritis, and it is the major reason for hospital admission [6, 14].
The golden standard for the assessment of the severity of dehydration is the percentage loss in body weight [1, 5, 6, 10, 14, 15], as measured by the difference between weight on admission and at 2 weeks after discharge, divided by weight at 2 weeks after discharge. Several clinical scores have been developed [5, 10]. According to the clinical score of the American Academy of Pediatrics (AAP) [1], patients are classified into three subgroups: mild dehydration (3–5%), moderate dehydration (6–9%), and severe dehydration (>10%) [1, 6]. Clinical scores for dehydration tend to underestimate the severity of dehydration and show only moderate agreement between observers [6, 15].
It is recommended to perform laboratory tests in dehydrated children if intravenous rehydration therapy is started, if there are signs and symptoms of increased serum sodium and in circulatory shock [6, 12]. Variables that are correlated best with the percentage of weight loss are: bicarbonate, blood urea nitrogen, and low pH in combination with a high base excess [3, 6, 9, 10, 14, 15]. However, none of the laboratory tests studied and presented in literature today can accurately estimate the percentage of weight loss in a general pediatric practice [12].
In dehydration, the percentage of weight loss was directly associated with the percentage of plasma volume lost [4, 13]. It was, therefore, hypothesized that plasma water may reflect the severity of dehydration. In 1952, Katcher et al. [4] studied plasma water in infants with dehydration. Plasma water was low in dehydrated children but recovered soon after rehydration [7].
In this study, we evaluated plasma water as a diagnostic tool in the assessment of dehydration in children with acute gastroenteritis admitted to hospital with moderate to severe dehydration.
Methods
The study was approved by the Medical Ethics Committee of the Maasstad Hospital Rotterdam. Between March 2006 and June 2008, all patients with acute gastroenteritis and dehydration visiting the Emergency Department of the Maasstad Hospital Rotterdam were asked to participate in the study. Exclusion criteria were: underlying metabolic disorders (e.g., diabetes mellitus), diabetes insipidus, and renal disease. Severity of dehydration was estimated on the basis of clinical assessment according to the practice parameter of the AAP [1], consisting of the following variables: blood pressure, quality of pulses, heart rate, skin turgor, depth of fontanel, humidity of mucous membranes, depth of eyes, capillary refill time, mental status, urine output, and thirst. Total scores consisted of sum of all variables ranging from one to three per variable. Plasma water was determined using a dry weight method (Sartorius® Technologies B.V. Eindhoven, the Netherlands). The measurement takes 50 µL of heparin plasma and is completed in 3 min. The plasma was evaporated to dryness (constant weight) by infrared radiation. Before and during evaporation, the sample weight was measured by automated weighing. The percentage of initial water content was then calculated from the wet and dry weight. From every blood sample, the plasma water was calculated twice (duplo measurements). The coefficient of variation calculated from 50 measurements in duplicate is 0.5%. The following laboratory tests were performed: sodium, potassium, chloride, blood urea nitrogen (BUN), creatinine, and venous blood gas analysis.
After clinical assessment of the severity of dehydration, all patients were rehydrated in 12 h. Patients were weighed before treatment, after 12-h rehydration and daily until discharge and 2 weeks after discharge at the outpatient clinic of the Maasstad Hospital Rotterdam. The golden standard for dehydration was based on weight gain after rehydration (difference between weight on admission and at 2 weeks after discharge divided by weight at 2 weeks after discharge). Results of plasma water measurements in dehydrated patients were compared to plasma water measurements of healthy controls (n = 12), visiting the outpatient clinic for functional disorders.
Statistical analysis
Two-tailed Wilcoxon rank-sum test was used to test clinical variables (mental status, quality of pulses, quality of breathing, skin turgor, fontanel, mucous membranes, eyes, extremities, urine output, thirst, capillary refill time) with the percentage of weight loss (data not shown). Associations between continuous variables (all laboratory tests, including: plasma water, sodium, potassium, chloride, BUN, serum creatinine, and venous blood gas analysis) are investigated using Spearman correlation coefficients. P = 0.05 (two-sided) was considered the limit of significance.
Results
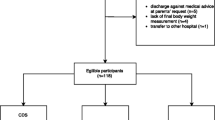
One hundred one patients (46 girls) were included in the study between March 2006 and June 2008. Demographic data of all 101 patients are listed in Table 1. Fifty-eight of patients were younger than 2 years of age, 32 were 2–5 years old, and 11 patients were older than 5 years. For 32 children, the percentage of weight loss could not be determined because of missing data. Demographic data of these 32 children did not differ from the total group (data not shown). According to the percentage of weight loss, 13/69 patients were slightly dehydrated (less than 3%), 18/69 were mildly dehydrated (3–5%), 12/69 moderately dehydrated (6–9%), and 26/69 severely dehydrated (more than 9%).
The median duration of admission was 3 days (range 1–10 days; Table 1). Duplo measurements of plasma water showed good reproducibility with an intraclass correlation of 0.95 (data not shown).
A decreased level of consciousnesses was significantly correlated with the percentage of weight loss (p < 0.05, two-tailed Wilcoxon rank-sum test). All other clinical signs did not significantly correlate with the percentage of weight loss (data not shown). Blood urea nitrogen (r = 0.3, p = 0.03, spearman correlation), base excess (r =−0.31, p = 0.03), and serum bicarbonate (r = 0.32, p = 0.02; Fig. 1) significantly correlated with the severity of dehydration.
Plasma water did not significantly correlate with the percentage of weight loss (r = 0.21, p = 0.98). In addition, no difference in plasma water levels was found between patients and healthy controls (Fig. 2).
Subgroup analysis showed that there was a trend towards a higher percentage of plasma water in moderate to severe dehydration (>6% weight loss).
Discussion
This is the first study in which plasma was measured in a large group of children with acute gastroenteritis and dehydration.
This study shows that clinical assessment of dehydration does not reflect the percentage of weight loss and that urea nitrogen, bicarbonate, and base excess are significantly correlated with the percentage of weight loss. These findings are in accordance with studies by others [3, 6, 9, 10, 12, 14, 15].
Plasma water was not correlated with the percentage of weight loss. Subgroup analysis showed that there was a trend towards a higher percentage of plasma water in moderate to severe dehydration (>6% weight loss).
How can we explain our findings on plasma water?
It is evident that plasma water is not a reliable measure to assess hydration status of children with acute gastroenteritis and dehydration. The physiological regulation of total body water and plasma water is complex and dynamic. Fluid balance is influenced by renal responses (e.g., arginine vasopressin) and by responses to vascular tonicity (e.g., aldosterone). It is evident from studies in experimental animals and in healthy humans that it takes some time for this complex regulatory system to find an equilibrium [2]. Hydration status can alter quickly in a response to rapid intake of a hypotonic fluid (e.g., water), and renal responses will protect against fluid overload (by producing hypo-osmolar urine). In addition, the body will respond to alterations in plasma osmolality. If initial fluid loss also results in electrolyte loss (like in acute gastroenteritis), the increase in plasma osmolality will be only moderate, which results in an attenuated mobilization of intracellular fluid to the plasma. Plasma water will increase more slowly accordingly. In addition, in a state of dehydration, rapid oral fluid intake can lead to rapid increase plasma water, before intracellular rehydration has started. We measured plasma water at one moment in time in children with acute gastroenteritis and dehydration, and probably none of these children’s fluid status was fully balanced. We, therefore, hypothesize that plasma water differs from child to child dependent of the actual fluid balance they are in the moment blood is drawn to measure plasma water. Factors like oral fluid and electrolyte intake, the amount of ongoing fluid—and electrolyte losses and differences in body size and composition—may have greatly influenced our results [2, 11].
Subgroup analysis showed that there was a trend towards a higher percentage of plasma water in children with moderate to severe dehydration. This result should be interpreted with caution. In theory, children with more severe dehydration are actually dehydrated longer, and they may have had time to mobilize more intracellular fluid to the plasma. More research is needed to find evidence for this hypothesis.
In accordance with the recent guideline commissioned by the National Institute for Health and Clinical Excellence [8], laboratory tests should not be routinely used. Laboratory tests should only be performed in case of intravenous rehydration therapy, clinical evidence for hypernatremia, and/or circulatory shock.
On the basis of our investigations, we conclude that there is insufficient evidence to justify the use of plasma water as a diagnostic tool in the assessment of dehydration in children with acute gastroenteritis.
References
American Academy of Pediatrics, Provisional Committee on Quality Improvement, Subcommittee on Acute Gastroenteritis (1996) Practice parameter: the management of acute gastro-enteritis in children. Pediatrics 97:424–435
Armstrong LE (2007) Assessing hydration status. The elusive gold standard. J Am Coll Nutr 26:575S–584S
Bonadia W, Hennes H, Machi J, Madagame E (1989) Efficacy of measuring BUN in Assessing children with dehydration due to gastro-enteritis. Ann Emerg Med 18:755–757
Czackes J (1961) Plasma volume as an index of total fluid loss. Am J Dis Child 102:190–193
Gorelick M, Shaw K, Murphy K (1997) Validity and reliability of clinical signs in the diagnosis of dehydration in children. Pediatrics 99(5):6
Guarino A, Albano F, Ashkenazi S et al (2008) ESPGHAN/ESPID evidence-based guidelines for the management of acute gastroenteritis in children in Europe Expert Working Group. J Pediatr Gastroenterol Nutr 46:619–621
Katcher A, Levitt M, Sweet A, Hodes H (1952) Studies of body-water distribution in normal infants during dehydration and subsequent recovery. Am J Dis Child 84(6):744–747
Khanna R, Lakhanpaul M, Burman-Roy S, Murphy MS, Guideline Development Group and the technical team (2009) Diarrhoea and vomiting caused by gastroenteritis in children under 5 years: summary of NICE guidance. BMJ 338:b1350
Kingston M (1973) Biochemical disturbances in breast-fed infants with gastro-enteritis and dehydration. J Pediatr 82:1073–1081
MacKenzie A, Barnes G, Shann F (1989) Clinical signs of dehydration. Lancet 2:605–607
Nose H, Mack GW, Shi X, Nadel ER (1988) Shift in body fluid compartments after dehydration in humans. J Appl Physiol 65(1):318–324
Shaoul R, Okev N, Lanir A, Jaffe M (2004) Value of laboratory studies in assessment of dehydration in children. Ann Clin Biochem 41:192–196
Steiner M, de Walt D, Byerley J (2004) Is this child dehydrated? JAMA 291:2746–2754
Teach SJ, Yates EW, Feld LG (1997) Laboratory predictors of fluid deficit in acutely dehydrated children. Clin Pediatr 36:395–400
Vega R, Avner J (1997) A prospective study of the usefulness of clinical and laboratory parameters for predicting percentage of dehydration in children. Pediatr Emerg Care 13:179–182
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Plaisier, A., Maingay-de Groof, F., Mast-Harwig, R. et al. Plasma water as a diagnostic tool in the assessment of dehydration in children with acute gastroenteritis. Eur J Pediatr 169, 883–886 (2010). https://doi.org/10.1007/s00431-010-1140-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-010-1140-8