Abstract
Purpose
This study compared cardiac computed tomography (CT) and two-dimensional transthoracic echocardiography (ECC) for assessing left ventricular ejection fraction (LVEF) using real-world data from a large patient population.
Materials and methods
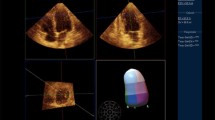
We studied 450 patients (284 males; mean age 64±12 years; range 12–88) who underwent CT and ECC due to suspected coronary artery disease. For CT, we used multiphase short-axis reconstructions and evaluated them with a dedicated software tool that uses Simpson’s rule to compute LV volumes. For ECC, computation was based on the biplane Simpson’s method. Results in terms of EF were compared with the paired Student’s t test, Pearson’s correlation coefficient (r), and Bland-Altman analysis.
Results
EF was 52%±15% for CT and 55%±13% for ECC. Statistically significant differences, albeit with good correlation, were observed between the measurements (r=0.71; p<0.05). ECC showed a slight tendency to overestimate EF. When the population was divided into subgroups according to EF, this was underestimated by ECC in the subgroup with EF >50% and overestimated in those with EF 35%–50% and <35%, with consistently significant differences between ECC and CT (p<0.05) and progressively lower levels of agreement.
Conclusions
In the real-world assessment of EF, ECC provides significantly different data from CT, with a bias that increases proportionally to LV systolic dysfunction.
Riassunto
Obiettivo
Obiettivo di questo studio è stato quello di confrontare la tomografia computerizzata (TC) del cuore con l’ecocardiogramma trans-toracico 2D (ECC) nel valutare la frazione di eiezione (FE) del ventricolo sinistro (Vsin) in una vasta popolazione di pazienti utilizzando dati provenienti dal mondo reale.
Materiali e metodi
Abbiamo incluso 450 pazienti (284 uomini; età media 64±12 anni; 12–88) che sono stati sottoposti a TC e a ECC per sospetta malattia coronarica; per la TC abbiamo utilizzato delle ricostruzioni multifasiche secondo un piano asse corto e le abbiamo valutate con un software dedicato, basato sul calcolo dei volumi del Vsin con la regola di Simpson; per l’ECC abbiamo utilizzato un calcolo basato sulla regola di Simpson biplanare. I risultati ottenuti per la FE sono stati analizzati con un test t di Student a due code per dati appaiati, una correlazione r di Pearson ed una analisi di Bland-Altman.
Risultati
La FE è stata 52%±15% per la TC e 55%±13% per l’ECC. Sono state osservate differenze statisticamente significative, anche se con buona correlazione, tra le misurazioni effettuate (r=0,71; p<0,05). L’ECC ha mostrato una lieve tendenza a sovrastimare la FE. Dividendo la nostra popolazione in sotto-gruppi, la FE è stata sottostimata dall’ECC nel sotto-gruppo con valori di FE>50%, ed è stata sovrastimata nei sotto-gruppi con FE compresa tra 35% e 50% ed in quello con FE<35%, con differenze tra TC ed ECC che si sono rivelate sempre significative (p<0,05) con una concordanza progressivamente più bassa.
Conclusioni
L’ECC fornisce valori di FE che sono significativamente differenti rispetto alla TC nel mondo reale, con un bias che aumenta proporzionalmente alla disfunzione sistolica del ventricolo sinistro.
Similar content being viewed by others
References/Bibliografia
Moise A, Bourassa MG, Theroux P et al (1985) Prognostic significance of progression of coronary artery disease. Am J Cardiol 55:941–946
Emond M, Mock MB, Davis KB et al (1994) Long-term survival of medically treated patients in the Coronary Artery Surgery Study (CASS) registry. Circulation 90:2645–2657
Juergens KU, Fischbach R (2006) Left ventricular function studied with MDCT. Eur Radiol 16:342–357
de Feyter PJ, van Eenige MJ, Dighton DH et al (1982) Prognostic value of exercise testing, coronary angiography and left ventriculography 6–8 weeks after myocardial infarction. Circulation 66:527–536
Taylor GJ, Humphries JO, Mellits ED et al (1980) Predictors of clinical course, coronary anatomy and left ventricular function after recovery from acute myocardial infarction. Circulation 62:960–970
White HD, Norris RM, Brown MA et al (1987) Left ventricular end-systolic volume as the major determinant of survival after recovery from myocardial infarction. Circulation 76:44–51
No authors listed (1983) Risk stratification and survival after myocardial infarction. N Engl J Med 309:331–336
Corbett JR, Dehmer GJ, Lewis SE et al (1981) The prognostic value of submaximal exercise testing with radionuclide ventriculography before hospital discharge in patients with recent myocardial infarction. Circulation 64:535–544
Shaw LJ, Peterson ED, Kesler K et al (1996) A meta-analysis of predischarge risk stratification after acute myocardial infarction with stress electrocardiographic, myocardial perfusion, and ventricular function imaging. Am J Cardio 178:1327–1337
Bansal D, Singh RM, Sarkar M et al (2008) Assessment of left ventricular function: comparison of cardiac multidetector-row computed tomography with two-dimension standard echocardiography for assessment of left ventricular function. Int J Cardiovasc Imaging 24:317–325
Pouleur AC, le Polain de Waroux PB, Pasquet A et al (2008) Assessment of left ventricular mass and volumes by three- dimensional echocardiography in patients with or without wall motion abnormalities: comparison against cine magnetic resonance imaging. Heart 94:1050–1057
Heuschmid M, Rothfuss JK, Schroeder S et al (2006) Assessment of left ventricular myocardial function using 16-slice multidetector-row computed tomography: comparison with magnetic resonance imaging and echocardiography. Eur Radiol 16:551–559
Nicol ED, Stirrup J, Reyes E et al (2008) Comparison of 64-slice cardiac computed tomography with myocardial perfusion scintigraphy for assessment of global and regional myocardial function and infarction in patients with low to intermediate likelihood of coronary artery disease. J Nucl Cardiol 15:497–502
Wua YW, Tadamuraa E, Yamamuroa M et al (2008) Estimation of global and regional cardiac function using 64-slice computed tomography: a comparison study with echocardiography, gated-SPECT and cardiovascular magnetic resonance. Int J Cardiol 128:69–76
Stegger L, Heijman E, Schäfers KP et al (2009) Quantification of left ventricular volumes and ejection fraction in mice using PET, compared with MRI. J Nucl Med 50:132–138
Sugeng L, Mor-Avi V, Weinert L et al (2006) Quantitative assessment of left ventricular size and function side-byside comparison of real-time three-dimensional echocardiography and computed tomography with magnetic resonance reference. Circulation 114:654–661
Puesken M, Fischbach R, Wenker M et al (2008) Global left-ventricular function assessment using dual-source multidetector CT: effect of improved temporal resolution on ventricular volume measurement. Eur Radiol 18:2087–2094
Salm LP, Schuijf JD, de Roos A et al (2006) Global and regional left ventricular function assessment with 16-detector row CT: comparison with echocardiography and cardiovascular magnetic resonance. Eur J Echocardiogr 7:308–314
Palumbo A, Maffei E, Martini C et al (2009) Functional parameters of left ventricle: comparison between cardiac mr and cardiac CT in a large population. Radiol Med, in press
Jenkins C, Moir S, Chan J et al (2009) Left ventricular volume measurement with echocardiography: a comparison of left ventricular opacification, threedimensional echocardiography, or both with magnetic resonance imaging. Eur Heart J 30:98–106
Chuang ML, Hibberd MG, Salton CJ et al (2000) Importance of imaging method over imaging modality in noninvasive determination of left ventricular volumes and ejection fraction: assessment by two- and three-dimensional echocardiography and magnetic resonance imaging. J Am Coll Cardiol 35:477–484
Cademartiri F, Maffei E, Notarangelo F et al (2008) 64-slice computed tomography coronary angiography: diagnostic accuracy in the real world. Radiol Med 113:163–180
Cademartiri F, La Grutta L, Palumbo A et al (2008) Computed tomography coronary angiography vs. stress ECG in patients with stable angina. Radiol Med 114:513–523.
Cademartiri F, Maffei E, Palumbo A et al (2007) Diagnostic accuracy of 64-slice computed tomography coronary angiography in patients with low-to-intermediate risk. Radiol Med 112:969–981
Cademartiri F, La Grutta L, Palumbo A et al (2007) Imaging techniques for the vulnerable coronary plaque. Radiol Med 112:637–659
Cademartiri F, Seitun S, Romano M et al (2008) Prognostic value of 64-slice coronary angiography in diabetes mellitus patients with known or suspected coronary artery disease compared with a nondiabetic population. Radiol Med 113:627–643
Cademartiri F, Romano M, Seitun S et al (2008) Prevalence and characteristics of coronary artery disease in a population with suspected ischaemic heart disease using CT coronary angiography: correlations with cardiovascular risk factors and clinical presentation Radiol Med 113:363–372
Lorenz CH, Walker ES, Morgan VL et al (1999) Normal human right and left ventricular mass, systolic function, and gender differences by cine magnetic resonance imaging. J Cardiovasc Magn Reson 1:7–21
Runza G, La Grutta L, Alaimo V et al (2008) Influence of heart rate in the selection of the optimal reconstruction window in routine clinical multislice coronary angiography. Radiol Med 113:644–657
Belge B, Coche E, Pasquet A et al (2006) Accurate estimation of global and regional cardiac function by retrospectively gated multidetector row computed tomography. Comparison with cine magnetic resonance imaging. Eur Radiol 16:1424–1433
Miller S, Simonetti OP, Carr J et al (2002) MR imaging of the heart with cine true fast imaging with steady-state precession: influence of spatial and temporal resolutions on left ventricular functional parameters. Radiology 223:263–269
van Geuns RJM, Baks T, Gronenschild EH et al (2006) Automatic quantitative left ventricular analysis of cine MR images by using three-dimensional information for contour detection. Radiology 240:215–221
Sievers B, Kirchberg S, Bakan A et al (2004) Impact of papillary muscles in ventricular volume and ejection fraction assessment by cardiovascular magnetic resonance. J Cardiovasc Magn Reson 6:9–16
Henry WL, DeMaria A, Gramiak R, King DL (1980) Report of the American Society of Echocardiography Committee on nomenclature and standards in two-dimensional echocardiography. Circulation 62:212–217
Lang RM, Bierig M, Devereux RB et al (2005) Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, Developed in Conjunction with the European Association of Echocardiography, a Branch of the European Society of Cardiology. J Am Soc Echocardiogr 18:1440–1463
Moss AJ, Zareba W, Hall WJ et al (2002) Prophylactic implantation of a defibrillator in patients with myocardial infarction and reduced ejection fraction. N Engl J Med 346:877–883
Moss AJ, Hall WJ, Cannom DS et al (1996) Improved survival with an implanted defibrillator in patients with coronary disease at high risk for ventricular arrhythmia. N Engl J Med 335:1933–1940
Bigger Jr JT, Fleiss JL, Kleiger R et al (1984) The relationships among ventricular arrhythmias, left ventricular dysfunction, and mortality in the 2 years after myocardial infarction. Circulation 69:250–258
Parameshwar J, Keegan J, Sparrow J et al (1992) Predictors of prognosis in severe chronic heart failure. Am Heart J 123:421–426
Bonow RO, Carabello B, de Leon Jr AC et al (1998) Guidelines for the management of patients with valvular heart disease: executive summary. A report of the American College of Cardiology/American Heart Association Task Force on practice guidelines (committee on management of patients with valvular heart disease). Circulation 98:1949–1984
Palazzuoli A, Cademartiri F, Geleijnse ML et al (2008) Left ventricular remodelling and systolic function measurement with 64 multi-slice computed tomography versus second harmonic echocardiography in patients with coronary artery disease: A double blind study. Eur J Radioly, in press. DOI:10.1016/j.ejrad.2008.09.022
Hendel RC, Patel MR, Kramer CM, at al. (2006) ACCF/ACR/SCCT/SCMR/ASNC/NASCI/SCAI/SIR 2006 appropriateness criteria for cardiac computed tomography and cardiac magnetic resonance imaging: a report of the American College of Cardiology Foundation Quality Strategic Directions Committee Appropriateness Criteria Working Group, American College of Radiology, Society of Cardiovascular Computed Tomography, Society for Cardiovascular Magnetic Resonance, American Society of Nuclear Cardiology, North American Society for Cardiac Imaging, Society for Cardiovascular Angiography and Interventions, and Society of Interventional Radiology. J Am Coll Cardiol 48:1475–1497
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maffei, E., Messalli, G., Palumbo, A. et al. Left ventricular ejection fraction: real-world comparison between cardiac computed tomography and echocardiography in a large population. Radiol med 115, 1015–1027 (2010). https://doi.org/10.1007/s11547-010-0542-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-010-0542-z